The Silent Thief of Bone Health

Each of us has a unique perspective on what health and “healthy aging” look like. Largely, many factors, such as genetic risk, access to good healthcare, or even zip code are out of our control. One important factor for managing health in aging depends on the ability to maintain some important reserves in the body. You could think of this like a retirement or savings account for which early or excessive withdrawal poses a risk to financial health later in life.
Bone and muscle, collectively referred to as the musculoskeletal (MSK) system, are examples of important reserves in the body that are often overlooked or unknowingly being depleted. In the case of bone, too often people are surprised when they are diagnosed with low bone density or osteoporosis only after a sudden fracture.
Described as a “silent disease” because you don’t feel your bones getting weaker, osteoporosis is a serious condition that is plagued with being neglected in screening and consequently underdiagnosed and undertreated. But, a woman’s risk of fracture is equal to her combined risk of breast, uterine, and ovarian cancer. And, for an estimated one in two women over the age of 50 who will suffer from an osteoporotic fracture, it can lead to a significant negative impact on their quality of life.
What is the “silent thief”?
Eating disorders, dieting, low body weight, and major weight loss are all risk factors recognized for stealing and whittling away at bone. Smoking, excess caffeine, and alcohol intake are also behaviors that can lead to consequences for long-term bone health.
Osteoporosis is a progressive, chronic disease in which the bone becomes thin, brittle, and fragile. Osteoporosis-related fractures – referred to as fragility fractures – can result from low-stress activities such as closing a window, bending over, coughing, lifting a box, or a simple fall from a standing height.
In fact, according to the International Osteoporosis Foundation, nearly 80% of individuals at high risk have already had at least one osteoporotic fracture before they are identified or treated for the disease.
These fractures are much more than an inconvenience. Vertebral fractures, for example, are one of the most common and are associated with severe pain, impaired lung function, difficulty in activities of daily living, slower walking pace, difficulty dressing, climbing stairs, and decreased independence – all leading to a significant negative impact on quality of life and increased mortality risk.
Prevention
Taking all of this into consideration, awareness and prioritizing prevention need to be a top priority in women’s health.
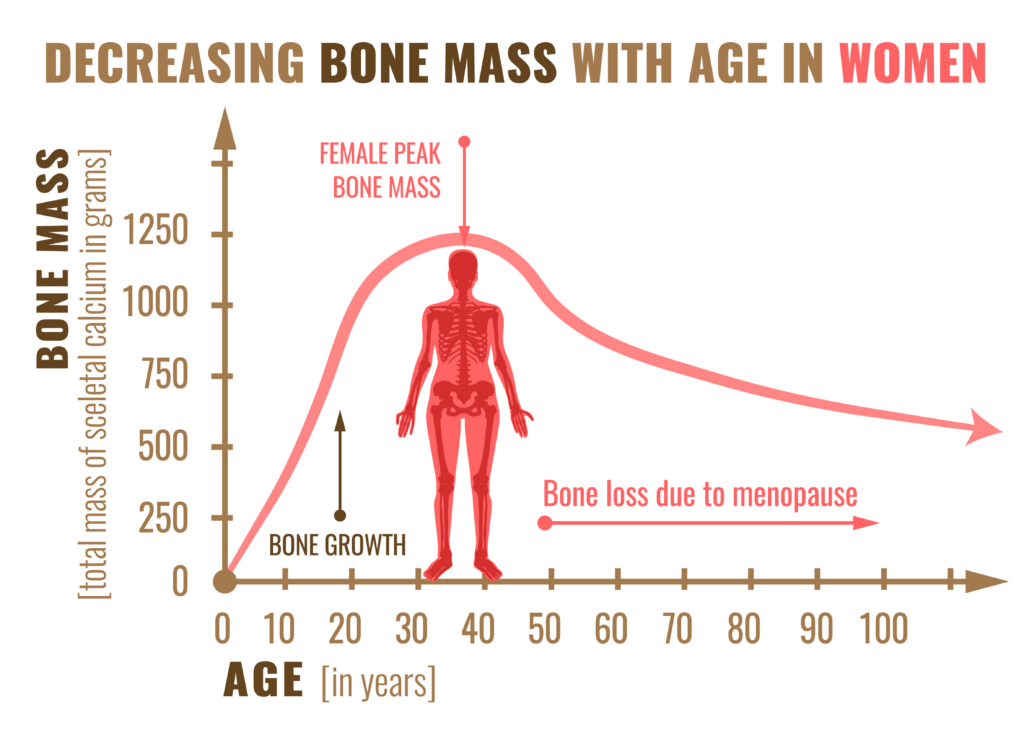
An individual’s peak bone mass is achieved by approximately age 25 and is largely determined by genetic factors, but is also impacted by nutrition, physical activity, and other factors related to health during growth and development. An adult’s skeleton is maintained by a process of bone remodeling where old bone is removed and replaced with new bone. Bone loss occurs when this balance is altered, and more bone is removed than is replaced.
Estrogen has a protective role in the bone remodeling process. Therefore, women are susceptible to low bone density during the menopause transition in which there is a rapid acceleration in bone loss that continues for a few years after the final menstrual period, resulting in as much as a 10-20% decrease in bone density before slowing to about 0.5 to 1% loss per year. Other conditions can also result in reduced estrogen levels, such as amenorrhea due to disordered eating, female athlete triad, or relative energy deficiency in sport (REDs). Therefore, treatment interventions are often aimed at restoring estrogen.
The Problem with Weight Loss
The loss of bone density due to weight loss is tragically overlooked and minimized in healthcare.
The TEMPO diet trial, by Seimon et al in 2019, illustrated the harmful impact of a 4-month “severe” diet intervention followed by an 8-month “moderate” calorie-restricted diet on bone mineral density. By the end of the 12-month trial, 40% of dieters in the “severe” group had developed osteopenia, despite weight stabilization after the fourth month, and all participants experienced significant loss of lean body mass. Similarly, a 2021 study, by Serra and Ryan, demonstrated that bone loss continues after weight loss, despite weight regain.
Weight loss delivers a double whammy to MSK health due to the loss of lean or skeletal tissue, which is vital for enabling strength and mobility. Muscle is also essential for maintaining mechanical resistance on bone, which in turn contributes to bone strength (as long as adequate nutrition is provided). Although resistance exercise and physical activity are meaningful interventions to attenuate lean tissue loss, trials that have demonstrated the intensity and level of the intervention necessary are likely not what most postmenopausal women with osteoporosis can sustain.
The plethora of studies, such as these, provide clear evidence that if diets and weight loss recommendations were treated like FDA-approved drugs, these “weight loss prescriptions” would require a “black box warning”.
A black box warning is the FDA’s most stringent warning for drugs and medical devices to alert the public and healthcare providers to serious side serious, permanent, or fatal side effects.
Screening and Diagnosis
Typically, there are no symptoms of osteoporosis, however, back pain, loss of height, a stooped posture, or a bone that breaks more easily than would be expected may be warning signs that should be investigated. Therefore, women are encouraged to speak with their doctors to understand how they can prevent or intervene sooner, rather than later, with monitoring their bone health.
Treatment and Managing Osteoporosis
Although there is no cure, osteoporosis is treatable with pharmaceutical interventions that can help maintain or enhance bone. Lifestyle interventions, such as nutrition and exercise can help slow the loss of bone and help prevent fractures. But the idea that you can “reverse” osteoporosis with nutrition, exercise, or things like supplementing with prunes is not correct and frankly could cause harm by delaying essential treatment interventions.
Nutrition and Exercise Interventions to Reduce Risk
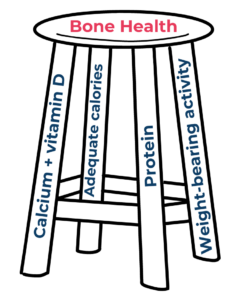 Bone health requires several key macro- and micronutrients along with adequate calorie intake to promote bone metabolism and support general physiology. The 4-legged stool pictured here illustrates the importance of these key components. Just like a wobbly and unstable stool would result if we removed any single one of the legs, the same is true when it comes to providing all the necessary ingredients for maintaining bone.
Bone health requires several key macro- and micronutrients along with adequate calorie intake to promote bone metabolism and support general physiology. The 4-legged stool pictured here illustrates the importance of these key components. Just like a wobbly and unstable stool would result if we removed any single one of the legs, the same is true when it comes to providing all the necessary ingredients for maintaining bone.
Adequate energy availability. Your body needs adequate energy intake to build bone – and reduce bone loss. Eating regular meals and snacks is important for delivering key nutrients and “fueling” the processes that go into metabolizing bone tissue.
Calcium. For women after age 50, 1200 milligrams (mg) per day is recommended from calcium-rich foods. In general, two excellent sources of calcium (i.e. milk, yogurt and cheese) plus 2-3 “good” sources of calcium (i.e. beans, tofu, almonds, oranges, broccoli) each day is a reasonable strategy for providing the recommended daily calcium. These calcium-rich foods have good bioavailability and many also contain protein and phosphorus to support overall bone health. The International Osteoporosis Foundation has a calcium calculator and is a fabulous resource overall. If supplemental calcium is recommended, it’s best to split doses of supplemental calcium so that you are taking no more than 500 mg at one time. Unlike natural sources of calcium from food, the body is unable to absorb more than that amount at one time.
Vitamin D. Adequate vitamin D levels, which are achieved through a combination of sunlight exposure, diet, and supplementation, are also important in bone health. As a general recommendation, 25(OH)D levels should be greater than 20 ng/mL. The ideal reference range is debated in the literature, but generally, between 30 and 50 ng/mL is recommended by the Vitamin D Council and National Osteoporosis Foundation. If supplementation is warranted, 1000 to 2000 IU of Vitamin D3 daily may be necessary to achieve the recommended levels in the body.
Protein. Protein provides part of the organic matrix of bone, and it can also have an indirect effect on the bone through its support for muscle mass and function. To date, expert consensus groups recommend 0.6 to 0.7 grams per pound of body weight per day from high-quality protein-containing foods, such as chicken, beef, fish, soy, beans, nuts, and dairy foods. If you are considering a protein supplement, it’s recommended to consider a complete protein, such as whey protein isolate, or soy and pea protein are plant-based alternatives.
Additional vitamins and minerals. There are numerous micronutrients, such as magnesium and vitamin K, that have a role in bone metabolism. A food-first approach helps to ensure adequate intake of all these nutrients.
Physical activity. The most important thing here is to try and avoid a sedentary lifestyle. An “ideal” exercise prescription would include enjoyable weight-bearing/resistance activity, 2-3 days per week, and balance and aerobic exercise on most days. But let’s be real. Stressors like aging parents, travel, family issues, illness, injury, or other mobility concerns, along with night sweats, sleep disturbances, or issues like osteoarthritis can impact a woman’s ability, energy, and/or time to be able to participate in activity. So, we need to give ourselves some space for compassion and realistic expectations regarding exercise. Remember that cleaning, gardening, raking the leaves, and other daily activities are also helpful. If you have been diagnosed with osteoporosis, I recommend working with a knowledgeable physical therapist who can guide you with appropriate exercises that will not set you up for injury or increased fracture risk.
Reduce Falls. Finally, apart from medications, diet, and exercise, it’s important to reduce the risk of falling. Changing to slip-proof footwear and rugs, reorganizing your living space to remove obstacles, and improving lighting can all be meaningful ways to reduce fracture risk and maintain health in aging.
How to Use This Information
I’m keenly aware that information like this can be tricky. On the one hand, it seems important to have the knowledge and awareness to help prevent disease and improve health outcomes. On the other hand, this type of information can often feel like a setup for one more thing that we need “to do” and sometimes it can feel impossible to “get it right.”
So, here are a few key takeaways:
- If you are concerned because you have had a history of an eating disorder or dieting, try to use this information as an opportunity to challenge your eating disorder and/or urges to diet or fixate on weight.
- If you have been diagnosed with osteoporosis, I encourage you to discuss treatment options with a qualified physician or endocrinologist. As recent as the 1970s, there were no medical interventions available for treating osteoporosis. Today, many treatment options are available and have rigorous and long observational studies to demonstrate efficacy as well as the benefits over risks. It’s disheartening to see postings from fitness influencers encouraging women to rely on weightlifting (and nutrition) instead of medication interventions for managing osteoporosis. Look, it’s your decision, but those recommendations do not align with best practices or standards of care from The Menopause Society, The International Menopause Society, or the International Osteoporosis Foundation.
- I encourage you to take in what is helpful, and leave behind or process with a therapist/dietitian the parts that worry you or that you need support with.
Back to our retirement account illustration. Imagine if we found out that our IRA was slowly being drained without our knowledge, that would stink. But, as soon as we learned about the problem, we would have an opportunity to take appropriate action to manage the situation and get back on track with our future goals.

With nearly two decades of experience as a registered dietitian, I’ve gained a deep understanding of the unique health challenges faced by women as they age, particularly during menopause. I hope to help you embrace midlife with confidence and vitality, and to show you that with the right mindset and approach, aging can be a time of great empowerment and joy.

Ready to prioritize your midlife health and wellness? The Four Pillars of Midlife Wellness will provide you with a fresh perspective on food, nutrition, health, and your body, enabling you to embrace your full potential and cultivate a robust sense of well-being throughout midlife and beyond!